TALAS™ (Torque Ankle Lever Arm System)
TALAS™ is a new hindfoot alignment measurement for weight bearing CT datasets.
A precise pre-operative measurement of hindfoot misalignment is paramount to surgical planning and post-operative follow-up. Weight bearing CT imaging is evolving our understanding of how to evaluate for alignment because it overcomes numerous measurement errors encountered by standard posterior weight bearing radiographs1.
TALAS™ (Torque Ankle Lever Arm System) (Patent No. 10/646137) is a software algorithm developed with the help of leading foot & ankle surgeons that can be used to automatically calculate hindfoot alignment based on reproducible three-dimensional anatomical landmarks. TALAS™ introduces the concept of 3D-specific biometric measurements, as opposed to 2D biometrics (ex. tibia-calcaneus angle) that are subject to projection and rotation error. A 3D biometric that TALAS proposes is Foot Ankle Offset (FAO). Peer-reviewed published studies demonstrate FAO is a reliable hindfoot measurement tool1 and can successfully quantify the risk of chronic lateral ankle instability2.
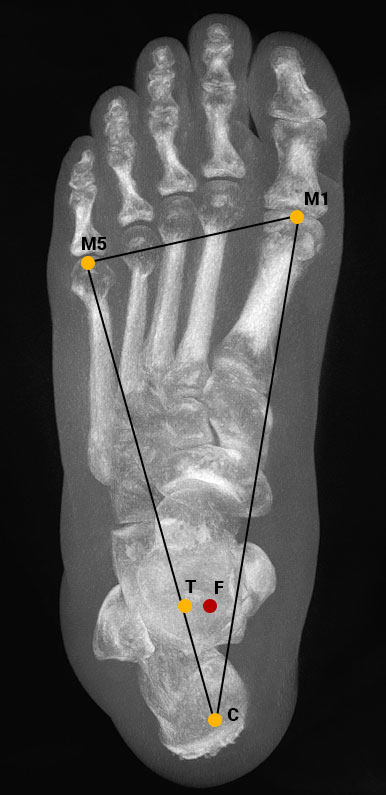
Using the TALAS™ tool in CubeVue, the user selects four anatomical landmarks: the most plantar weight bearing point of the first metatarsal (M1), the fifth metatarsal (M5), the calcaneal weight bearing area (C) and the center-most point of the ankle joint (D). The landmarks are recorded as coordinates in a three-dimensional volume.
“Using weight bearing CT with Foot Ankle Offset to calculate a ‘safe zone’ for 3D alignment of the foot prior to a total ankle replacement procedure could be instrumental in preventing osteolysis, a condition which often leads to implant failure.”
-Dr. Francois Lintz, MD, FEBOT, winner of 2019 IFFAS Award of
Excellence for his research on residual mis-alignment in total ankle replacement patients.

TALAS uses a mathematical algorithm as defined by Dr. Francois Lintz et al.(2) to calculate:
Foot Ankle Offset (FAO)
The FAO represents the distance between where the center of the ankle joint projects on the ground and where the center of the gravity of the foot lies. FAO is given as a percentage of foot length rather than a distance, so that the results may be compared regardless of foot size. According to the initial data, the norm for this value is 2-3%, which corresponds to a slight valgus. This is in accordance with data gathered from 2D biometric studies.
Calcaneal Offset (CO)
Calcaneal offset is defined as the distance between a theoretically neutral position of the calcaneus (where FAO = 0%) and the actual position of the calcaneus (C’). The calcaneal offset is presented as a distance measurement (mm).
Hindfoot Angle (HA)
The hindfoot angle is included as a reference measurement for surgeons who may not be accustomed to working with offset calculations. The apex of the center of the talar dome projected on the ground plane (D) forms the vertex, and the ideal position of the calcaneus (C) an the actual position of the calcaneus (C’) form the endpoints of this angle.
Hindfoot Alignment
Hindfoot alignment is presented as a value on a scale in which the right-most value is -30 % and the left-most value is 30 %. A hindfoot with no varus or valgus will scale in the center, at 0%. A hindfoot in varus will scale between 0 and -30%. The position of the presentation reflects, in %, the degree of varus. Conversely, a hindfoot in valgus will scale between 0 and 30 %.
(1) “Measuring hindfoot alignment in weight bearing CT: A novel clinical relevant measurement method”. Burssens, A. et al. Foot and Ankle Surgery, Volume 22, Issue 2, Supplement 1, Page 24
(2) “Ground Reaction Force Calcaneal Offset: A new measurement of hindfoot alignment”. Lintz, F. et al. Foot and Ankle Surgery, Volume 18, Issue 1. Foot and Ankle Surgery, Volume 0, Issue 0.
(3) “The hindfoot alignment view”. Saltzman C. et al. Foot Ankle Int. 1995 Sep; 16(9):572-6.


